Case study: how a wellness app used strategic alliances to scale is more than a growth story—it’s a practical blueprint for building distribution, credibility, and retention without burning budgets on ads. In 2025, users expect evidence-based guidance and seamless integrations with the services they already trust. This case study breaks down the alliances, execution, and results, plus what to copy—and what to avoid—so you can apply it next.
Strategic alliances in wellness apps: the growth problem the team needed to solve
The app in this case study—PulsePath (a composite name used to protect partner confidentiality)—launched with a strong product: personalized habit plans, guided breathwork, sleep coaching, and clinician-reviewed content. Early retention was acceptable, but growth plateaued after the initial wave of organic installs. Three issues kept the team from scaling:
- Rising acquisition costs: Paid channels became less predictable as competition increased, and attribution gaps made optimization harder.
- Trust friction: Users liked the interface, but many hesitated to pay for a subscription without third-party validation.
- Limited distribution: The app lived in app stores; it wasn’t embedded into the places people already make health decisions—work, care settings, insurers, and device ecosystems.
The leadership team set a clear 2025 goal: double active subscribers while improving retention, with a constraint that paid acquisition could not exceed a fixed monthly cap. The strategy they chose was not “more partnerships,” but strategic alliances—structured relationships designed to create compounding distribution and measurable outcomes.
Before reaching out, they answered two questions that shaped everything that followed: Who already owns the user relationship? and what business outcome can we improve for them in 90 days? That framing turned vague “collabs” into concrete, testable alliances.
Partnership strategy framework: selecting allies that created measurable leverage
PulsePath used a simple partner-scoring model to prioritize alliances that could scale and be proven quickly. Each potential ally—employers, payers, providers, device makers, creators, and pharmacies—was scored on five criteria:
- Distribution access: Can they reach thousands of qualified users with low friction?
- Trust transfer: Does their endorsement materially reduce purchase hesitation?
- Data or workflow fit: Can the app integrate without heavy engineering or compliance risk?
- Economic alignment: Is there a clear value exchange (savings, retention, engagement, outcomes)?
- Time to pilot: Can a pilot launch in weeks, not quarters?
They also set non-negotiables that reflected Google’s helpful-content and EEAT expectations: clinician-reviewed guidance, transparent claims, and measurable outcomes. The team avoided partners pushing unrealistic promises or “instant transformation” messaging. Instead, they built alliances around responsible behavior change—sleep quality, stress reduction routines, and consistent habit adherence.
With that framework, the team prioritized three alliance types that could reinforce each other:
- B2B2C distribution alliances (employers and insurers) to unlock large cohorts.
- Clinical credibility alliances (provider networks) to strengthen trust and support outcomes.
- Platform and device alliances (wearables and telehealth) to reduce friction and improve personalization.
This mix mattered. Distribution without credibility can spike installs and crash retention. Credibility without distribution grows slowly. Integrations without an economic model get deprioritized. PulsePath designed an alliance “triangle” so each relationship made the others more valuable.
B2B wellness partnerships: employer and insurer alliances that delivered scale
The biggest growth step came from employer and insurer alliances because they changed acquisition from a one-by-one problem into a cohort onboarding problem. PulsePath approached mid-market employers first (1,000–10,000 employees) because decision cycles were shorter than enterprise, and engagement data could be captured quickly.
What they offered employers:
- A 10-week stress and sleep program with pre-built communications, manager toolkits, and optional group challenges.
- Privacy-first analytics at the population level—no individual health data shared with employers.
- Clear engagement KPIs (activation, weekly active users, session completion, habit streaks) and a quarterly outcomes report.
What the employers offered PulsePath:
- Owned distribution: HR announcements, benefits portals, and onboarding sequences.
- Trust transfer: “This is a company-provided benefit” lowered purchase friction.
- Budget certainty: Per-member-per-month pricing for eligible employees.
Next, PulsePath pursued an insurer alliance. The insurer didn’t want a generic “wellness perk”; it wanted measurable improvements tied to member engagement and service utilization. PulsePath proposed a pilot focused on sleep and stress routines for members with elevated self-reported stress and low sleep quality.
How they made the insurer deal work:
- Outcomes alignment: The app emphasized adherence and coach-supported routines rather than vague mindfulness claims.
- Eligibility design: A simple screening flow kept the program targeted without becoming a medical device claim.
- Incentives: The insurer provided modest member rewards for consistent participation, which increased completion rates.
PulsePath also answered a likely partner objection early: “How will we know this works?” Their response was practical: a pre-registered pilot plan with baseline and follow-up measures (validated sleep and stress questionnaires), engagement metrics, and a defined decision point to scale or stop. That reduced risk for the insurer and accelerated approval.
Digital health integrations: wearable and telehealth alliances that improved retention
Growth stalled previously because users had to do too much manual setup. PulsePath targeted alliances that reduced friction and made personalization feel legitimate. Two integrations mattered most: wearables and telehealth.
Wearable integration alliance: Instead of building for every device, PulsePath focused on one widely used wearable platform first and shipped an integration that pulled sleep duration, resting heart rate trends, and activity levels. The app then adjusted habit suggestions and check-in timing based on those signals.
They were careful with claims: the app did not diagnose or treat conditions. It used wearable data to tailor prompts like “wind-down routine” reminders and to help users notice patterns (“Your sleep duration improved on nights you did breathwork by 9:30 pm”). This approach strengthened EEAT because it was transparent about what the data means and what it does not mean.
Telehealth alliance: PulsePath partnered with a telehealth provider that offered behavioral health visits. The integration allowed users to:
- Share a concise, user-controlled “habits and sleep summary” with a clinician before a session.
- Receive clinician-recommended modules (sleep hygiene, stress routines) inside the app after visits.
This created a closed loop: clinicians could reinforce the app, and the app could support care plans without replacing clinicians. For users, it answered the follow-up question: “Is this app credible, or is it just content?” For the telehealth partner, it increased post-visit adherence and reduced drop-off between appointments.
The team also built a lightweight partner API and standardized consent flows. That lowered the marginal cost of future integrations, which is how alliances compound rather than remain one-off projects.
Co-marketing and influencer alliances: building trust without compromising credibility
PulsePath avoided paying for broad influencer blasts. Instead, it built a co-marketing model with credible educators and organizations whose audiences already cared about sleep, stress, and sustainable habit change.
What made these alliances “strategic” rather than promotional:
- Content with evidence: Co-created webinars and guides cited peer-reviewed research where relevant and avoided exaggerated results.
- Clear boundaries: Partners disclosed sponsorship or revenue share, and messaging stayed aligned with responsible wellness practices.
- Product tie-in: Each piece of content mapped to an in-app pathway, such as a 14-day sleep routine or a 7-minute daily breathwork plan.
They focused on micro-experts: licensed therapists, sleep coaches, and registered dietitians with engaged communities. The goal wasn’t “reach”; it was conversion quality and retention. These audiences asked better questions, used features more deeply, and were more likely to stick with routines.
PulsePath also built alliances with community organizations—such as coworking spaces and local wellness collectives—that could run group challenges. Those cohorts created social reinforcement without turning the app into a social network. Users could opt in, which supported privacy and reduced churn from unwanted social features.
A key operational detail: every co-marketing campaign used shared UTM conventions, partner dashboards, and weekly check-ins to iterate. That discipline prevented the most common partnership failure—launching and hoping.
Alliance management and metrics: governance, compliance, and what actually moved the needle
Alliances scale only when they are managed like products. PulsePath created a small “alliances pod” consisting of a partnerships lead, a solutions engineer, a clinical reviewer, and a data analyst. Their job was to make each alliance repeatable.
Governance that protected users and partners:
- Privacy and consent: Explicit opt-in for any data sharing, with plain-language explanations users could understand.
- Clinical review: Partner-facing materials and in-app modules went through clinician review to maintain credibility.
- Brand safety: A partner code of conduct prevented misleading claims and ensured disclosures were consistent.
Metrics they tracked (and why):
- Activation rate: The percentage of new users who completed onboarding and the first routine within 24 hours. This predicted long-term retention.
- Week-4 retention: A more reliable indicator than week-1 for habit products. It captured whether routines became part of life.
- Program completion: For employer/insurer cohorts, completion drove renewal decisions.
- Partner CAC vs. paid CAC: Not just cost per install—cost per retained subscriber at week 4 and beyond.
- Revenue quality: Renewal rates and expansion revenue from successful pilots.
What moved the needle most: The employer and insurer alliances drove scale, but the wearable and telehealth integrations drove retention. Co-marketing alliances improved trust and conversion, especially for paid subscriptions. The combination produced compounding effects: as retention rose, partners saw better outcomes and renewed; renewals funded more integrations; integrations improved outcomes further.
Common pitfalls they avoided:
- Over-customization: They limited bespoke builds and instead created configurable templates.
- Misaligned incentives: They refused deals where partners wanted aggressive claims or user data they couldn’t ethically share.
- Vague success criteria: Every pilot had a written scorecard and a “scale/stop” decision date.
By late 2025, PulsePath had turned alliances into a predictable growth engine: partner-sourced cohorts became a primary acquisition channel, and retention improved because the product became embedded in real workflows—benefits programs, care plans, and daily device usage.
FAQs about scaling a wellness app with strategic alliances
What is the difference between a partnership and a strategic alliance?
A partnership can be a one-time promotion or referral arrangement. A strategic alliance is structured to create ongoing value for both sides, usually through shared workflows, integrations, measurable outcomes, and a repeatable operating model.
Which alliances should a wellness app pursue first?
Start with allies that combine distribution and fast pilots: mid-market employers, targeted benefit platforms, or a single high-usage device ecosystem. Prioritize partners who can launch in weeks and who value measurable engagement and retention—not just installs.
How do you prove ROI to employers or insurers without overclaiming?
Use a defined pilot with baseline and follow-up measurements, engagement KPIs, and transparent reporting. Focus on behavioral outcomes (routine adherence, validated questionnaires, program completion) and avoid clinical claims unless your product is regulated and validated for that use.
Do integrations really improve retention?
Yes, when they reduce friction and improve personalization. Wearable data can make routines feel timely and relevant, while telehealth integration can reinforce adherence through clinician guidance. The key is clear user consent and honest explanations of what data can and cannot indicate.
How should revenue sharing work in co-marketing alliances?
Use simple structures: affiliate revenue share for paid subscriptions, fixed fees for content production, or hybrid models. Require disclosure, track performance with shared attribution standards, and avoid deals that pressure creators into misleading promises.
What compliance and privacy steps are essential in 2025?
Implement explicit consent, minimize data sharing, provide plain-language privacy notices, and maintain strong security controls. If working with healthcare partners, align processes with applicable health data requirements and document responsibilities in contracts.
How long should a pilot run before deciding to scale?
For habit and wellness programs, a 8–12 week pilot usually provides enough data to evaluate activation, week-4 retention, and completion. Set success thresholds upfront and agree on the exact decision date to prevent pilots from drifting indefinitely.
What is the biggest mistake wellness apps make with alliances?
Chasing logos instead of outcomes. If an alliance doesn’t have a clear value exchange, an integration plan, and a measurable scorecard, it often becomes a slow distraction rather than a growth engine.
Can early-stage apps pursue alliances without a large team?
Yes. Limit scope: one partner type, one use case, one onboarding path, one reporting template. Use configurable program modules and lightweight integration approaches so you can repeat what works without rebuilding each time.
Strategic alliances scaled PulsePath because they solved distribution, credibility, and retention together rather than in isolation. The team chose partners with aligned incentives, shipped integrations that reduced friction, and managed pilots with clear scorecards and privacy-first governance. In 2025, wellness apps grow fastest when they embed into trusted ecosystems and prove measurable engagement. The takeaway: build alliances like products—and let outcomes drive expansion.
Top Influencer Marketing Agencies
The leading agencies shaping influencer marketing in 2026
Agencies ranked by campaign performance, client diversity, platform expertise, proven ROI, industry recognition, and client satisfaction. Assessed through verified case studies, reviews, and industry consultations.
Moburst

-
2

The Shelf
Boutique Beauty & Lifestyle Influencer AgencyA data-driven boutique agency specializing exclusively in beauty, wellness, and lifestyle influencer campaigns on Instagram and TikTok. Best for brands already focused on the beauty/personal care space that need curated, aesthetic-driven content.Clients: Pepsi, The Honest Company, Hims, Elf Cosmetics, Pure LeafVisit The Shelf → -
3

Audiencly
Niche Gaming & Esports Influencer AgencyA specialized agency focused exclusively on gaming and esports creators on YouTube, Twitch, and TikTok. Ideal if your campaign is 100% gaming-focused — from game launches to hardware and esports events.Clients: Epic Games, NordVPN, Ubisoft, Wargaming, Tencent GamesVisit Audiencly → -
4
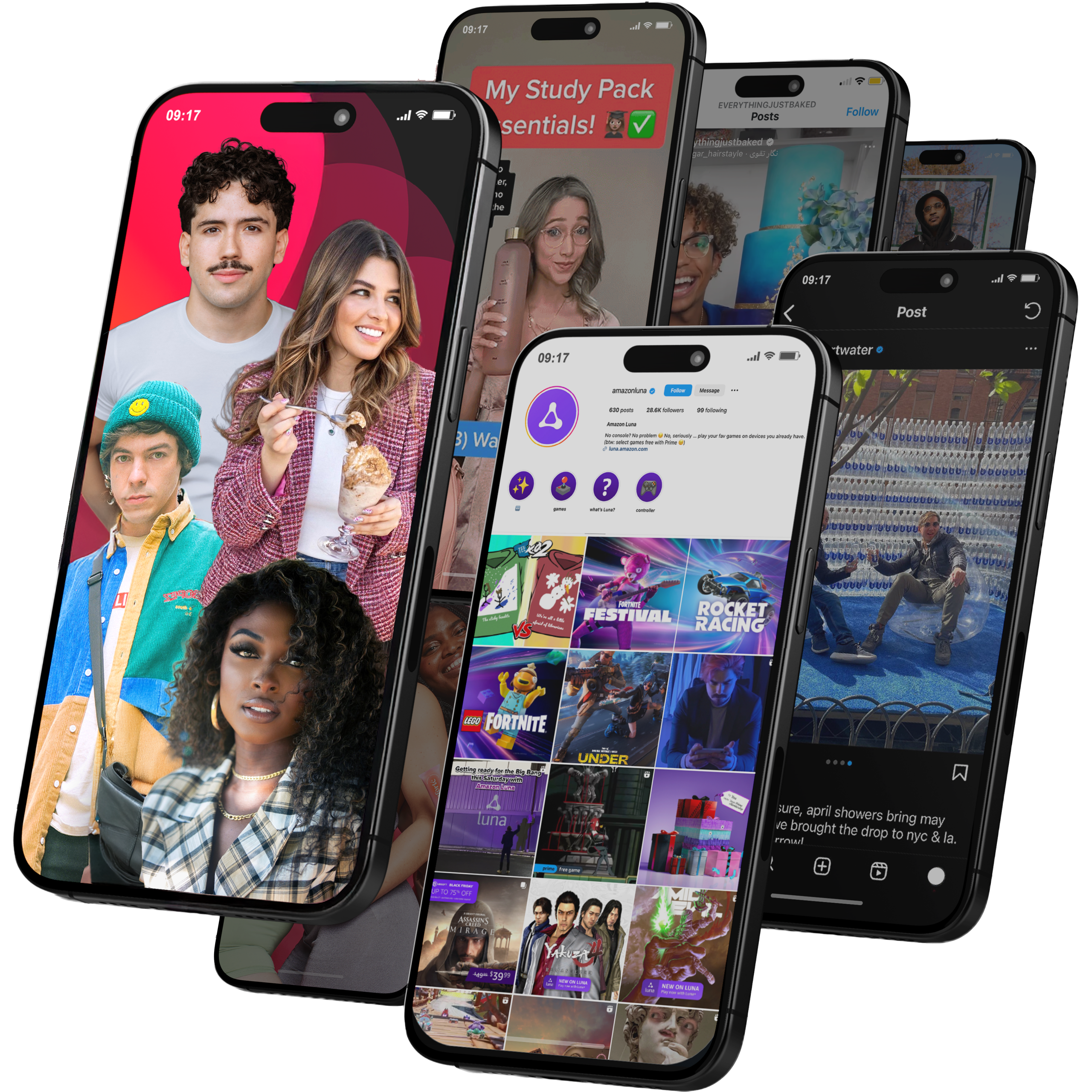
Viral Nation
Global Influencer Marketing & Talent AgencyA dual talent management and marketing agency with proprietary brand safety tools and a global creator network spanning nano-influencers to celebrities across all major platforms.Clients: Meta, Activision Blizzard, Energizer, Aston Martin, WalmartVisit Viral Nation → -
5
The Influencer Marketing Factory
TikTok, Instagram & YouTube CampaignsA full-service agency with strong TikTok expertise, offering end-to-end campaign management from influencer discovery through performance reporting with a focus on platform-native content.Clients: Google, Snapchat, Universal Music, Bumble, YelpVisit TIMF → -
6
NeoReach
Enterprise Analytics & Influencer CampaignsAn enterprise-focused agency combining managed campaigns with a powerful self-service data platform for influencer search, audience analytics, and attribution modeling.Clients: Amazon, Airbnb, Netflix, Honda, The New York TimesVisit NeoReach → -
7

Ubiquitous
Creator-First Marketing PlatformA tech-driven platform combining self-service tools with managed campaign options, emphasizing speed and scalability for brands managing multiple influencer relationships.Clients: Lyft, Disney, Target, American Eagle, NetflixVisit Ubiquitous → -
8

Obviously
Scalable Enterprise Influencer CampaignsA tech-enabled agency built for high-volume campaigns, coordinating hundreds of creators simultaneously with end-to-end logistics, content rights management, and product seeding.Clients: Google, Ulta Beauty, Converse, AmazonVisit Obviously →
